2026 PPS Lifetime Achievement Award
William D. Travis, MD
PPS 2026 - Registration now available!
Register now - PPS Biennial Dinner!
2026 PPS Biennial Meeting Program (pdf)
Hotel Accomodations
Meeting venue: Palais Montcalm
Abstract submission closed
June 27 1:00 - 4:00 PM (last day)
Additional Session: International Mesothelioma Panel (all PPS members welcome!)
At main venue. Free - No additional Cost
See Program
March Case of the Month Clinical History:
A 30-year-old woman presented with a 7-day history of fever, cough, shortness of breath, and hemoptysis. She had short stature, microcephaly, dysmorphism with coarse facies , puffy eyes and thin telangiectatic skin. Seven months prior she was diagnosed as sarcoidosis based on her previous CT and high ACE levels and she was treated with prednisolone, mycophenolate, and azathioprine.
Current CT chest showed diffuse smooth lobular and interlobular septal thickening with GGOs in bilateral lungs (crazy paving pattern ) and multiple bilateral mediastinal lymphadenopathy CECT abdomen was done and it showed hepatosplenomegaly. Her lipid profile showed reduced HDL cholesterol (21 mg/dL), increased total cholesterol (194 mg/dL), and non-HDL cholesterol (176 mg/dL); CRP was increased. All other investigations including CBC, RFT, LFT, malarial parasite, blood cultures, and autoimmune profile were negative; her vitals and SpO2 were normal; 2D echo was normal.
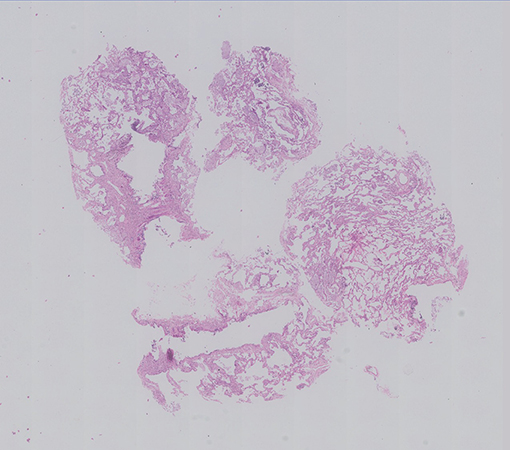
An EBUS guided Cryo lung biopsy and mediastinal lymph node biopsy were done along with Bronchial washings and sent for histopathological examination. Her BAL Infectious workup (bacterial, fungal, mycobacterial ) was negative. The cryobiopsy showed multiple fragments of tissue showing alveolated lung parenchyma with preserved architecture (Fig 1). Many clusters of foamy macrophages are noted in the alveolar spaces; they are variable in size, show multiple fine vacuoles in the cytoplasm with some of them showing deep blue granules (Fig 2). They are seen in the interstitium (Fig 3) as well as in the bronchovascular bundles. The alveolar interstitium is widened by moderate mononuclear inflammatory infiltrate and mild interstitial fibrosis.(Fig 2, 3). The bronchiolar epithelial cells are vacuolated, (Fig 3), however the Type II pneumocytes appear normal or show focal mild reactive atypia (Fig 2). No other significant pathological changes are identified.The pulmonary vasculature was unremarkable.
The mediastinal lymph node biopsy (Fig 4,5) and the bronchial wash cell block (Fig 6) also showed similar clusters of foamy macrophages A PAS and a PAS-D stains were done and the foamy macrophages were negative (Fig 7).
Based on the above histological features a diagnosis of Endogenous lipoid pneumonia was offered raising the possibility of Acid sphingomyelinase deficiency disease (ASMD). Enzyme activity assays and Genetic mutational studies were suggested for confirmation of the same..
Click here to see more.
A 30-year-old woman presented with a 7-day history of fever, cough, shortness of breath, and hemoptysis. She had short stature, microcephaly, dysmorphism with coarse facies , puffy eyes and thin telangiectatic skin. Seven months prior she was diagnosed as sarcoidosis based on her previous CT and high ACE levels and she was treated with prednisolone, mycophenolate, and azathioprine.
Current CT chest showed diffuse smooth lobular and interlobular septal thickening with GGOs in bilateral lungs (crazy paving pattern ) and multiple bilateral mediastinal lymphadenopathy CECT abdomen was done and it showed hepatosplenomegaly. Her lipid profile showed reduced HDL cholesterol (21 mg/dL), increased total cholesterol (194 mg/dL), and non-HDL cholesterol (176 mg/dL); CRP was increased. All other investigations including CBC, RFT, LFT, malarial parasite, blood cultures, and autoimmune profile were negative; her vitals and SpO2 were normal; 2D echo was normal.
An EBUS guided Cryo lung biopsy and mediastinal lymph node biopsy were done along with Bronchial washings and sent for histopathological examination. Her BAL Infectious workup (bacterial, fungal, mycobacterial ) was negative. The cryobiopsy showed multiple fragments of tissue showing alveolated lung parenchyma with preserved architecture (Fig 1). Many clusters of foamy macrophages are noted in the alveolar spaces; they are variable in size, show multiple fine vacuoles in the cytoplasm with some of them showing deep blue granules (Fig 2). They are seen in the interstitium (Fig 3) as well as in the bronchovascular bundles. The alveolar interstitium is widened by moderate mononuclear inflammatory infiltrate and mild interstitial fibrosis.(Fig 2, 3). The bronchiolar epithelial cells are vacuolated, (Fig 3), however the Type II pneumocytes appear normal or show focal mild reactive atypia (Fig 2). No other significant pathological changes are identified.The pulmonary vasculature was unremarkable.
The mediastinal lymph node biopsy (Fig 4,5) and the bronchial wash cell block (Fig 6) also showed similar clusters of foamy macrophages A PAS and a PAS-D stains were done and the foamy macrophages were negative (Fig 7).
Based on the above histological features a diagnosis of Endogenous lipoid pneumonia was offered raising the possibility of Acid sphingomyelinase deficiency disease (ASMD). Enzyme activity assays and Genetic mutational studies were suggested for confirmation of the same..
Click here to see more.