Click here to see all images
June, 2017
Case of the Month
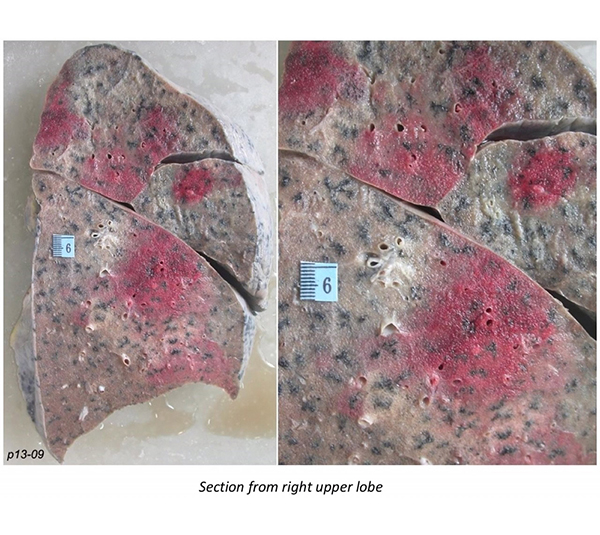
Clinical History:A 40-year-old post-menopausal woman presented with intermittent fever, chills, body ache, easy fatigability, and generalized weakness for two months. She was found to have pancytopenia with a few atypical cells (myeloblast morphology). The patient worsened clinically and expired within two days of admission. At autopsy, blasts were seen within the bone marrow, liver and spleen. The gross morphology of the right lung and sections from the right upper lobe are shown in Figures 1-6.
Quiz:
Q1. In tissue, which of the following fungi form septate hyphae with narrow-angle branching?
- Mucor, Absidia, Rhizopus
- Aspergillus, Candida, Blastomyces
- Pseudallescheria, Fusarium, Aspergillus
- Histoplasma, Cryptococcus, Pneumocystis
Q2. Which of the following is true?
- The halo sign is specific for aspergillosis.
- The halo sign is a ground-glass opacity surrounded by a solid rim.
- The halo sign is seen in angioinvasive fungal infections.
- The reverse halo sign is pathognomonic of organizing pneumonia.
Q3. What is an aspergilloma?
- A non-invasive fungus ball within a pre-existing cavity.
- A hypersensitivity reaction to Aspergillus in susceptible hosts, characterized by allergic mucin.
- A lesion formed by invasion of lung parenchyma by fungi, with granulomatous inflammation.
- A consequence of vascular invasion by fungal organisms.
Q4. Invasive aspergillosis most typically occurs in individuals with:
- Anemia
- Lymphocytopenia
- Neutrophilia
- Neutropenia
Answers to Quiz
Q1. C
Q2. C
Q3. A
Q4. D
Q2. C
Q3. A
Q4. D
Diagnosis
Angioinvasive fungal pneumonia
Discussion
Aspergillus is a ubiquitous fungus that can produce a wide spectrum of clinical features depending on factors such as the immune status of the host and the presence of underlying structural lung disease. The sinonasal tract and lungs are the most commonly involved sites, reflecting the portals of entry of the infectious asexual spores (conidia). The gastrointestinal tract and skin are less commonly involved. The term pulmonary aspergillosis encompasses allergic bronchopulmonary aspergillosis (a hypersensitivity reaction to fungi in asthmatic individuals), aspergilloma (non-invasive colonization of a preexisting pulmonary cavity by a fungus ball), chronic necrotizing aspergillosis (semi-invasive fungal infection accompanied by necrotizing granulomatous inflammation), and invasive/angioinvasive aspergillosis (invasion of blood vessels by fungal hyphae). Invasive aspergillosis develops in severely immunocompromised individuals (typically neutropenic patients with acute myeloid leukemia), critically ill patients, and patients taking corticosteroids. Neutrophil NADPH oxidase and activation of antimicrobial proteases constitute the most important host defences against fungal hyphae. Neutropenia (absolute neutrophil count less than 500/µL) for more than ten days is the most classic risk factor for invasive aspergillosis. The most typical radiologic finding of angioinvasive fungal infections is the “halo sign”, which is a solid nodule surrounded by a ground-glass opacity. This sign is not specific for aspergillosis.
Grossly, target lesions are characteristic of invasive aspergillosis. They are characterized by a zone of necrosis surrounded by a hemorrhagic rim (Figure 1). Microscopically they are comprised of a central zone of ischemic necrosis, surrounded by a zone of fibrinous exudate with neutrophils and a zone of parenchymal hemorrhage. An occluded necrotic artery can often be identified at the edge of the lesion. In the present case, the specimen retained an unfixed appearance in spite of perfusion fixation (Figure 1). Microscopically, Aspergillus forms septate hyphae that branch at acute/narrow angles (Figures 2, 4, 5, and 6). Fruiting bodies (spore-bearing structures) may be present if the organisms are in contact with air, as in an aspergilloma or a bronchopleural fistula. Although the majority of septate fungal hyphae with narrow-angle branching in the lung represent Aspergillus, this organism cannot be distinguished from morphologically similar fungi such as Pseudallescheria boydii and Fusarium based on histomorphology alone, and cultures are required for definitive identification. In the current case, since cultures could not be performed, we are using the term “invasive fungal pneumonia” rather than invasive aspergillosis.
The key pathologic finding in invasive aspergillosis (and other invasive fungal pneumonias) is invasion of blood vessels by fungal hyphae, often accompanied by thrombosis, which produces areas of hemorrhage and infarction. In the present case there was a lack of inflammation, and infarct-like necrosis was seen in the absence of thrombotic occlusion. Serum galactomannan is a useful laboratory test for invasive aspergillosis, and voriconazole is the antifungal agent of choice.
Take home message: In the lung, septate fungal hyphae with narrow-angle branching are not always Aspergillus.
Grossly, target lesions are characteristic of invasive aspergillosis. They are characterized by a zone of necrosis surrounded by a hemorrhagic rim (Figure 1). Microscopically they are comprised of a central zone of ischemic necrosis, surrounded by a zone of fibrinous exudate with neutrophils and a zone of parenchymal hemorrhage. An occluded necrotic artery can often be identified at the edge of the lesion. In the present case, the specimen retained an unfixed appearance in spite of perfusion fixation (Figure 1). Microscopically, Aspergillus forms septate hyphae that branch at acute/narrow angles (Figures 2, 4, 5, and 6). Fruiting bodies (spore-bearing structures) may be present if the organisms are in contact with air, as in an aspergilloma or a bronchopleural fistula. Although the majority of septate fungal hyphae with narrow-angle branching in the lung represent Aspergillus, this organism cannot be distinguished from morphologically similar fungi such as Pseudallescheria boydii and Fusarium based on histomorphology alone, and cultures are required for definitive identification. In the current case, since cultures could not be performed, we are using the term “invasive fungal pneumonia” rather than invasive aspergillosis.
The key pathologic finding in invasive aspergillosis (and other invasive fungal pneumonias) is invasion of blood vessels by fungal hyphae, often accompanied by thrombosis, which produces areas of hemorrhage and infarction. In the present case there was a lack of inflammation, and infarct-like necrosis was seen in the absence of thrombotic occlusion. Serum galactomannan is a useful laboratory test for invasive aspergillosis, and voriconazole is the antifungal agent of choice.
Take home message: In the lung, septate fungal hyphae with narrow-angle branching are not always Aspergillus.
References
Kosmidis C, Denning DW. The clinical spectrum of pulmonary aspergillosis. Thorax 2015;70:270-7.
Kousha M, Tadi R, Soubani AO. Pulmonary aspergillosis: a clinical review. Eur Respir Rev 2011;20:156-74.
Patterson KC, Strek ME. Diagnosis and treatment of pulmonary aspergillosis syndromes. Chest 2014;146:1358-68.
Raju S, Ghosh S, Mehta AC. Chest computed tomography signs in pulmonary disease – a pictorial review. Chest. 2017 Jun;151(6):1356-1374.
Segal BH. Aspergillosis. N Engl J Med 2009;360:1870-
Kousha M, Tadi R, Soubani AO. Pulmonary aspergillosis: a clinical review. Eur Respir Rev 2011;20:156-74.
Patterson KC, Strek ME. Diagnosis and treatment of pulmonary aspergillosis syndromes. Chest 2014;146:1358-68.
Raju S, Ghosh S, Mehta AC. Chest computed tomography signs in pulmonary disease – a pictorial review. Chest. 2017 Jun;151(6):1356-1374.
Segal BH. Aspergillosis. N Engl J Med 2009;360:1870-
Contributors
Saranya Singaravel, DCP, DNB (Path)
Pradeep Vaideeswar, MD (Path)
Department of Pathology, Cardiovascular and Thoracic Division,
Seth GS Medical College and KEM Hospital, Mumbai, India
Pradeep Vaideeswar, MD (Path)
Department of Pathology, Cardiovascular and Thoracic Division,
Seth GS Medical College and KEM Hospital, Mumbai, India