Click here to see all images
September, 2020
Case of the Month
Clinical History: A 52-year-old man presented to the emergency room with a history of recent-onset shivers, nausea and headache. He worked in construction and excavation. He had a history of dyslipidemia, was a non-smoker, and did not use drugs. There was no recent travel history and no exposure to birds. He was found to be tachycardic and febrile, with an elevated white blood cell count dominated by neutrophils. Pulmonary examination was unremarkable, with an O2 saturation of 92% by pulse oximetry. Screening for SARS-COV-2 was negative. Chest x-ray and CT scan showed bilateral ground-glass and reticulonodular opacities. He was treated empirically with broad-spectrum antibiotics while awaiting results of microbiological cultures, without improvement. Induced sputum culture returned positive for “filamentous fungus suggestive of Aspergillus spp”. While there was some suspicion this might have been a contaminant, antifungals were added to the antibiotics. With little clinical improvement and an unclear diagnosis, the decision was taken to perform a surgical lung biopsy for histopathologic diagnosis.
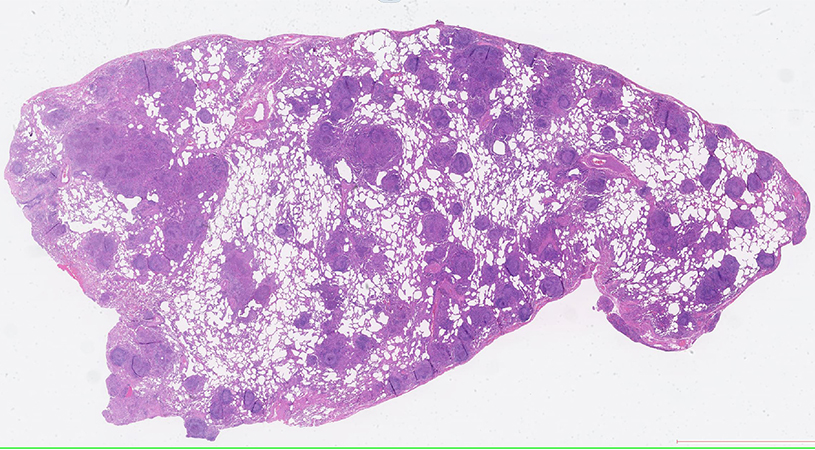
The biopsies correlated with the radiologic images, showing a diffuse micronodular pattern characterized by innumerable interstitial granulomas. The granulomas were diffusely distributed, without apparent predilection for centrilobular, paraseptal or subpleural zones, and did not directly involve vessels (Fig 1). The granulomas were well formed, with a dense neutrophilic (suppurative) center associated with fibrin and basophilic debris, surrounded by a rim of epithelioid histiocytes and occasional giant cells (Fig 2, 3). They occasionally involved small airways with ulceration of the bronchiolar epithelium and extension of the granulomatous inflammation into the airway lumen (Fig 4). In some granulomas, fragmented branching hyphal structures could be seen (Fig 5). These structures were positive on GMS (Fig 6). No other microorganisms were visible with other special stains.
Quiz:
Q1. Pulmonary infection with which of the following microorganisms is typically associated with suppurative granulomas?
- Aspergillus fumigatus
- Blastomyces dermatitidis
- Mycobacterium tuberculosis
- Coccidioides immitis
Q2. Which of the following are manifestations of Aspergillus in the lung of an immunocompetent person?
- Allergic bronchopulmonary aspergillosis
- Chronic cavitary/necrotizing aspergillosis
- Aspergilloma
- All of the above.
Q3. Which of the following are morphologic features of Aspergillus hyphae on histology:
- Acute angle branching
- Septation
- Between 2-6 µm wide
- All of the above
Answers to Quiz
Q2. D
Q3. D
Diagnosis
Discussion
As noted in the quiz, the typical clinicopathologic manifestations of Aspergillus in the immunocompetent patient include aspergilloma (non-granulomatous fungal colonization of a pre-existing cavity), allergic bronchopulmonary aspergillosis (allergic eosinophilic reaction to airway fungus in patients with asthma), and chronic cavitary/necrotizing aspergillosis (progressive cavitary necrotizing granulomas). The fourth and possibly most well-known manifestation is invasive aspergillosis which occurs in severely immunocompromised individuals, in which fungal hyphae are seen directly invading into parenchyma and vessel walls, with associated hemorrhagic necrosis and little to no inflammatory response.
With this in mind, we return to the present case, which, as you have likely surmised, is quite unusual. Aspergillus spp. is not typically associated with suppurative granulomas in the lung. As in any case in which the pathologic pattern is somewhat discordant with the presumed causative agent, one must ask oneself: is there anything else at play here? Why is this host reacting to this fungus in this way? While the clinical history is not particularly suggestive, the extent of disease certainly raises concern for an immunocompromised state. In this particular case, screening for HIV was negative, no blood lineage was suppressed, and serum immunoglobulins were within normal limits. A review of the literature revealed a few cases with a similar histologic pattern of diffuse suppurative granulomas associated with Aspergillus in otherwise healthy adults, who on further workup were found to have chronic granulomatous disease. Lo and behold, when genetic testing was performed on the patient in the current case, a homozygous deletion in the NCF1 gene was detected, confirming the diagnosis of chronic granulomatous disease. This disease is caused by deletion or inactivating mutations in one of five genes (CYBA, CYBB, NCF1, NCF2, NCF4) resulting in a dysfunctional NADPH-oxidase complex and failure to generate a proper phagocyte respiratory burst. While the majority of cases present in early life, it is known that some cases present late into adulthood, as exemplified by this case. Notably, Aspergillus remains the single most common infectious cause of death in patients with chronic granulomatous disease.
References
King J, Henriet SSV, Warris A. Aspergillosis in chronic granulomatous disease. J Fungi (Basel) 2016;2:1-16.
Mukhopadhyay S, Gal AA. Granulomatous lung disease: an approach to the differential diagnosis. Arch Pathol Lab Med 2010;134:667-90.
Shah KK, Pritt BS, Alexander MP. Histopathologic review of granulomatous inflammation. J Clin Tuberc Other Mycobact Dis 2017;7:1-12.
Williams D, Kadaria D, Sodhi A, et al. Chronic granulomatous disease presenting as Aspergillus fumigatus pneumonia in a previously healthy young woman. Am J Case Rep 2017;18:351-4.
Contributor
Thoracic Pathologist
University of Montreal Health Center
Montreal, Quebec, Canada